COVID-19 Guidelines
Last content update: 3/8/24
On January 9, 2024, the California Department of Public Health (CDPH) issued new isolation and quarantine recommendations for the general public to focus on protecting those most at risk for serious illness while reducing social disruption that is disproportionate to recommendations for the prevention of other endemic respiratory viral infections. The revised guidance recommends that people with COVID-19 isolate until they have been fever-free for at least 24 hours without the use of fever-reducing medications and their symptoms are mild and improving. The guidance also recommends that people with COVID-19 continue to mask around others and avoid contact with people at higher-risk of severe COVID-19 for a full 10 days.
As Santa Clara County moves to align with this new isolation guidance, the County Public Health Department wants our community to be aware that the best scientific information still indicates that individuals with COVID-19 may be infectious for around 10 days after they become sick or test positive. In addition, COVID-19 continues to cause more hospitalizations and deaths in Santa Clara County than either flu or RSV. Given this ongoing risk of COVID-19 transmission, in instances where the benefits outweigh the harms, individuals may consider using additional layers of protection when feasible, such as maximizing indoor ventilation and filtration, working remotely, and avoiding large indoor gatherings.
COVID-19 Guidelines
- Stay home if you have COVID-19 symptoms until you have been fever-free for 24 hours without using fever-reducing medicine AND other COVID-19 symptoms are mild and improving.
- If you do not have symptoms, you should still follow the recommendations below to reduce exposure to others.
- Mask when you are around other people indoors for 10 days after you become sick (or 10 days after you test positive, if you do not have symptoms).
- You may remove your mask sooner than day 10 if you test negative with an antigen test twice, with at least one day in between tests.
- Avoid contact with people at higher risk for severe COVID-19 for 10 days. This includes the elderly, those who live in congregate care facilities, and people with weak immune systems or medical conditions that put them at higher risk for serious illness.
If you have mild or moderate symptoms, a healthcare provider may decide you are eligible for COVID-19 treatment. Talk with your doctor as soon as possible about COVID-19 treatment if you are at higher risk of severe illness. Free treatment options are available, regardless of insurance or immigration status.
Do not delay seeking treatment for COVID-19 - it works best when given as soon as possible after testing positive.
Get medical help right away if you start feeling sicker, especially if you have trouble breathing, persistent chest pain, begin to feel confused, cannot stay awake, or develop bluish lips or face.
The Public Health Department wants our community to be aware that the best scientific information indicates that people with COVID-19 may be infectious for around 10 days after they become sick or test positive. In addition, COVID-19 continues to cause more hospitalizations and deaths in Santa Clara County than either flu or RSV. Given this ongoing risk of COVID-19 transmission, people who have COVID-19 may consider using additional layers of protection in the 10 days after becoming sick in situations where the benefits outweigh the harms. These additional layers of protection may include increasing indoor ventilation and filtration, working remotely, and avoiding large indoor gatherings.
- Wear a mask and get tested right away - visit the County’s testing webpage to find a testing site near you or get free at-home tests.
- While you are waiting for your COVID-19 test results, stay home until you have been fever-free for 24 hours without using fever-reducing medicine and other symptoms are improving.
- Watch your symptoms closely and get medical care if you feel worse, especially if you are at higher risk of serious illness.
If you test positive for COVID-19, follow the guidelines above.
If you test negative for COVID-19, you can return to normal activities once you have been fever-free for 24 hours (without use of fever-reducing medicine) and other symptoms are mild and improving. If you tested negative with an antigen test, you should test again at least a day later. If new symptoms develop, stay home and get tested again.
- Consider testing within 5 days after last close contact with a COVID-19 case and before contact with higher-risk people.
- If you are at higher risk for severe illness or have contact with people who are at higher risk for severe illness, you should get tested within 5 days after last exposure.
- Wear a mask indoors if you are around people at higher risk for severe illness in the 10 days after last close contact with a COVID-19 case.
Please note:
- The guidance above is aligned with California Department of Public Health’s guidelines. Refer to these guidelines for additional information about the above recommendations.
- In the workplace, employers are subject to the Cal/OSHA COVID-19 Prevention Non-Emergency Regulations or in some workplaces the Cal/OSHA Aerosol Transmissible Diseases (ATD) Standard, and should consult those regulations for additional applicable requirements.
- This guidance does NOT apply to healthcare providers or patients/residents in any kind of healthcare facility. For more information, see COVID-19 Resources for Providers.
Frequently Asked Questions
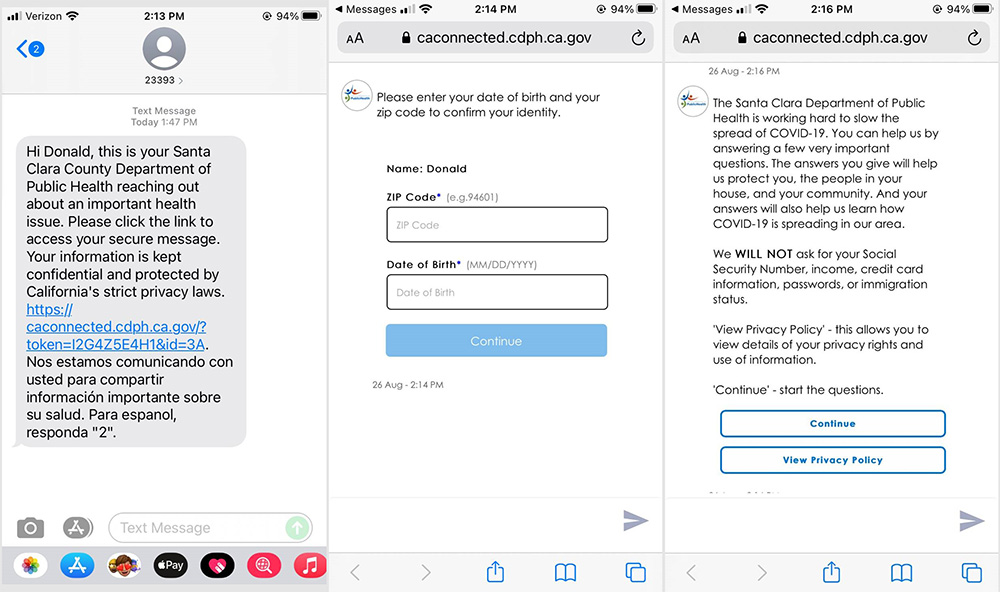
If you receive a text from the phone number 233-93 with a survey link, this is the County of Santa Clara Public Health Department contacting you to ask questions about how you are feeling and provide information about COVID-19 treatment and other resources. It is safe to click on the link in this text message.
Your privacy is incredibly important to us, and any information you provide will only be used by the Public Health Department to ensure the health and safety of our community. You will never be asked for your social security number, financial information, or immigration status.
Below are screenshots of what the text message and survey will look like:
Description: These images show the text message and survey you will receive from the County of Santa Clara Public Health Department.
For more information, see this video from CDPH.
A person who tests positive for COVID-19 and has symptoms is potentially contagious from 2 days before symptoms began until 10 days after symptoms began.
A person who tests positive for COVID-19 and does not have symptoms is potentially contagious from 2 days before the date of their first positive COVID-19 test until 10 days after the date of their first positive test.
The Public Health Department wants our community to be aware that the best scientific information indicates that people with COVID-19 may be infectious for around 10 days after they become sick or test positive. In addition, COVID-19 continues to cause more hospitalizations and deaths in Santa Clara County than either flu or RSV. For these reasons, people who have COVID-19 should follow all guidelines for people who test positive and may consider using additional layers of protection in the 10 days after becoming sick in situations where the benefits outweigh the harms. These additional layers of protection may include increasing indoor ventilation and filtration, working remotely, and avoiding large indoor gatherings.
For smaller indoor spaces (such as homes, clinic waiting rooms, or airplanes), anyone who was in the indoor space at the same time as someone who tested positive for COVID-19 and has symptoms for a total of 15 minutes or more during a 24-hour period is considered a close contact.
For large indoor spaces (such as large retail stores, warehouses, or indoor concert venues), anyone who was within 6 feet of a person who tested positive for COVID-19 and has symptoms for a total of 15 minutes or more in a 24-hour period is considered a close contact.
For more information, see the California Department of Public Health definition of “close contact”.
Some people are at higher risk for serious COVID-19 illness than others. Specifically, older adults, people who are immunocompromised, and people with underlying health conditions are more likely to develop more serious symptoms and to require more medical care, especially if they are unvaccinated.
For more information, visit the CDC’s People with Certain Medical Conditions webpage.
To learn more about COVID-19, visit the CDC’s COVID-19 Homepage or CDPH’s COVID-19 Resources webpage.
Guidance for Businesses and Workplaces
Businesses in Santa Clara County are responsible for taking steps to protect the health of their workers and customers. All businesses and workplaces in Santa Clara County are subject to the requirements in Cal/OSHA COVID-19 Prevention Non-Emergency Regulations, or in some workplaces the Cal/OSHA Aerosol Transmissible Diseases (ATD) Standard, and should consult those regulations for additional applicable requirements.
Face coverings must be worn at certain times and in certain settings as required by a County Health Order Requiring Use of Face Masks in Patient Care Areas of Health Care Delivery Facilities During Designated Winter Respiratory Virus Period and Cal/OSHA.
The guidance below does NOT apply to businesses and employers in healthcare settings.
For information on COVID-19-related requirements for healthcare facilities, refer to COVID-19 Resources for Providers.
See Cal/OSHA COVID-19 Prevention Non-Emergency Regulations and related FAQs for more information on employer requirements related to COVID-19 testing, exposure and isolation.
In the event a worker tests positive for COVID-19, employers must follow the requirements outlined in Cal/OSHA COVID-19 Prevention Non-Emergency Regulations or, if applicable, the Cal/OSHA Aerosol Transmissible Diseases (ATD) Standard.
Employers should also refer to the California Department of Public Health (CDPH) Responding to COVID-19 in the Workplace for Employers webpage for additional guidance.
The County of Santa Clara discourages employers from requiring a medical note from a doctor or healthcare provider for clearance to return to work after a worker has COVID-19.
Businesses and employers in non-healthcare settings must follow Cal/OSHA requirements, including requirements to report COVID-19 outbreaks to Cal/OSHA. For more information, refer to Cal/OSHA COVID-19 Prevention Non-Emergency Regulations and related FAQs.
Most non-healthcare businesses are no longer required by law to report COVID-19 cases or outbreaks among staff to the Public Health Department. However, businesses can voluntarily report large outbreaks of 20 or more cases by calling the Public Health Department’s Communicable Disease Prevention and Control Program at (408) 885-4214.
During an outbreak, additional layers of protection may be needed to halt transmission. It is important to identify and test all potentially exposed individuals regardless of their vaccination status. It is also important to review internal COVID-19 response plans, identify ongoing COVID-19 hazards at the workplace, and determine what additional mitigation steps may be needed.
If your business is experiencing an outbreak and you need support in understanding COVID-19 guidance or would like additional technical assistance from Public Health, please contact [email protected].
Guidance for Ventilation and Air Filtration Systems
Visit sccphd.org/saferair to learn how to improve indoor air at your business or refer to additional resources below.
- Interim Guidance for Ventilation, Filtration, and Air Quality in Indoor Environments (California Department of Public Health)
- Ventilation in Buildings (Centers for Disease Control)
- Best Practices for Ventilation of Isolation Areas in Skilled Nursing Facilities, Long-Term Care Facilities, Hospices, Drug Treatment Facilities, and Homeless Shelters (California Department of Public Health)
Additional Guidance and Resources
- Responding to COVID-19 in the Workplace (California Department of Public Health)
- Statewide Industry Guidance to Reduce Risk (California Department of Public Health)
- Cal/OSHA COVID-19 Guidance and Resources (California Division of Occupational Safety and Health)
- Labor & Workforce Development Agency (State of California)
- Employment Development Department (EDD) (State of California)
- COVID-19 Worker Benefits and Leave Navigator (State of California)
- sccfairworkplace.org (County of Santa Clara)
Guidance for Schools and Childcare
State of California Safe Schools for All Hub, including:
-
California Department of Public Health COVID-19 Isolation Guidance for the General Public
-
California Department of Public Health Guidance for K-12 Schools and Child Care Settings to Support Safe In-Person Services and Mitigate the Spread of Communicable Diseases, 2023-2024 School Year
-
California Department of Public Health Considerations when a Child has Symptoms of Illness in Child Care or School
-
California Department of Social Services COVID-19 FAQs for Licensed Childcare Facilities and Providers
- Schools and childcare providers shall promptly notify the Public Health Department when at least 5% of their school population - with a minimum of 5 ill among students and staff - have reported a suspected or confirmed COVID-19 infection over a 14-day period.
-
Schools are encouraged to use the Designee Reporting Calendar Spreadsheet to track the percentage of new suspected or new confirmed cases in their school population over 14 days. Watch a 7-minute tutorial on how to use the Designee Reporting Calendar.
-
To report COVID-19 cases:
-
If you do NOT have an existing SPOT account linked to the location you are reporting for, submit a SPOT Intake Form to report case information.
-
If you have an existing SPOT account linked to the location you are reporting for, you may report case information by logging into SPOT and reporting cases directly to the Location Account. Please click “Existing Users” to log in and navigate to the “Report Cases and Contacts” section of SPOT to submit new case information for the appropriate location from the drop-down list.
-
2. Cal/OSHA COVID-19 Prevention Non-Emergency Regulations.
3. Childcare providers must report outbreaks to their Regional Licensing Office.
An outbreak of COVID-19 is defined by CDPH as at least three confirmed COVID-19 cases reported within a 7-day period among people who are epidemiologically linked in the setting and are not known to be close contacts of each other in any other case investigation.
Ventilation and Air Quality
-
Ventilation in Schools and Childcare Programs (Centers for Disease Control)
-
ASHRAE Managing Air Quality During the Pandemic (American Society of Heating, Refrigerating, and Air-Conditioning Engineers)
Resources for Reporting to SPOT
-
For detailed instructions on submitting to SPOT, see SPOT School Help and Training Material.
-
For technical assistance with submission of SPOT Intake Forms (e.g., login or password assistance), please contact the SPOT Help Desk at [email protected] or (916) 520-1619.
-
If you have additional questions about outbreaks or reporting, please email [email protected].